Researchers at the University of Illinois at Urbana-Champaign and Washington University in St. Louis have developed a new device that may one day help prevent heart attacks.
Unlike existing pacemakers and implantable defibrillators that are one-size-fits-all, the new device is a thin, elastic membrane designed to stretch over the heart like a custom-made glove.
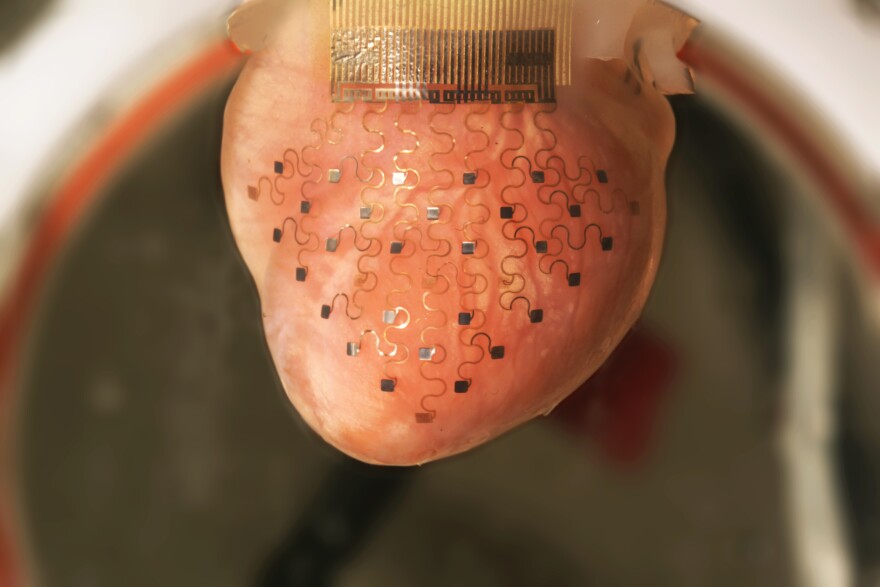
This video shows a rabbit heart that has been kept beating outside of the body in a nutrient and oxygen-rich solution. The new cardiac device -- a thin, stretchable membrane imprinted with a spider-web-like network of sensors and electrodes -- is custom-designed to fit over the heart and contract and expand with it as it beats. Credit: University of Illinois and Washington University.
University of Illinois materials scientist John Rogers co-led the team that invented the new device.
He says they used high-resolution imaging, computer modeling, and a 3-D printer to create a plastic model of a heart. Then, they used that as a mold to make a thin, elastic membrane designed to fit snugly over the real heart’s surface.
Rogers compares the silicon version to the heart’s natural membrane, the pericardium. “But this artificial pericardium is instrumented with high quality, man-made devices that can sense and interact with the heart in different ways that are relevant to clinical cardiology,” Rogers said.

Washington University biomedical engineer Igor Efimov helped design and test the new device.
He says the membrane’s spider-web-like network of specialized electrodes can continuously monitor the heart’s electrical activity and keep it beating at a healthy rate.
“When it senses such a catastrophic event as a heart attack or arrhythmia, it can also apply a high definition therapy,” Efimov said. “So it can apply stimuli, electrical stimuli, from different locations on the device in an optimal fashion to stop this arrhythmia and prevent sudden cardiac death.”
Efimov calls the new device a huge advance and hopes it will be approved for use in patients in 10 to 15 years.
Their research is published in the journal Nature Communications.
Follow Veronique LaCapra on Twitter: @KWMUScience